|
|
The “typical” canine lymphoma patient is a middle-aged dog brought to the veterinarian because one or more lumps have been found. The veterinarian rapidly determines that all of the peripheral lymph nodes (those near the skin surface) are enlarged and firm. Usually the dog has not been showing any signs of illness. The next step is a blood panel and urinalysis to more completely assess the patient’s health and one or more lymph nodes are aspirated or biopsied to confirm the diagnosis of lymphoma.
So here we are. We have confirmed lymphoma and we know the average life expectancy for a patient with untreated lymphoma is about 2 months from the time of diagnosis. If this is your dog you probably need some time to absorb the import of the cancer diagnosis. You have many general questions and you know that a decision regarding chemotherapy must be rendered.
We will attempt to cover commonly asked questions owners have at this point. |

|
|
How did my dog get lymphoma?
We do not know how
dogs (or people for that matter) get cancer most of the time.
There are many types of cancer and many possible causes of
cancer (chemicals in our environment, sun exposure, assorted
viruses and infections). There are important genetic factors
as well. Cancer starts with one or a small group of cells
that have “gone wrong.” It appears that such cells arise in
our bodies all the time and we have an assortment of natural
mechanisms to destroy these cells before they get out of hand.
Sometimes these cancer cells escape our natural mechanisms
and cancer develops. It is important to realize that cancer
is not contagious and that, as a pet owner, you should not
feel that you caused this or brought it on your pet somehow.
Many people feel a need to find blame and latch onto the idea
that a household cleaner or pesticide was the cause. This
is a natural part of grieving but it is important not to focus
on cause unduly. Cause is not relevant to treatment; further,
there is no way to verify cause. It is best to concentrate
on treatment. At this time, there is no way to know what caused
lymphoma development in a given patient.
Can my dog be cured?
Theoretically, yes,
but practically speaking no. It is best to focus on a realistic
outcome which is the longest possible survival with good quality
life. Different treatment protocols are associated with different
disease-free intervals.
|
|
Does my pet need further tests?
If a biopsy has not been performed, it is a good idea to have one done so as to gain the maximum information about the tumor (whether it is slow or fast growing, what type of lymphocytes are involved etc.) as this information can help predict the response to chemotherapy. In cats, due to the effects of the feline leukemia virus on the bone marrow, a biopsy is absolutely necessary to diagnose lymphoma as there are many other blood diseases that can mimic lymphoma. In the dog, however, a lymph node aspirate is frequently adequate to make the lymphoma diagnosis. Many oncologists will require a biopsy prior to referral.
Other tests that may be recommended include a bone marrow aspirate and/or a spleen or liver aspirate. These tests are needed to stage the disease. Lymphoma is classified by stage:
-
Stage I: - only one lymph node involved
-
Stage II: - several lymph nodes in the same general area involved
-
Stage III: - all peripheral lymph nodes involved
-
Stage IV: - all peripheral lymph nodes plus the spleen, liver, and/or anterior mediastinum in the chest involved
-
Stage V: - everything in stage IV plus bone marrow involvement
In cases of lymphoma that are not as straightforward as the classical multicentric lymphoma described above, staging may be more important. Staging used to be done regularly after the initial diagnosis of lymphoma but it has since been found that stage of disease does not impact upon the response to chemotherapy (i.e., it is not true that a stage II will have a better response than a stage IV). The exception is Stage V, the most advanced stage. Patients with stage V lymphoma tend to have a poor response to chemotherapy.
How does lymphoma cause death?
Lymphoma is a rapidly growing malignancy that is able to go and grow anywhere where there is lymph tissue. This is virtually every organ in the body. Eventually, the cancer will infiltrate an organ to such an extent that that organ fails (often this is the bone marrow or the liver). The patient loses his/her appetite, vomits or gets diarrhea, weakens and dies. At some point the tumor becomes resistant to therapy and no further remissions can be obtained.
My dog does not fit the above scenario at all. What are other forms of lymphoma?
Lymphoma is classified
by anatomic area affected. By far, the most common form in the dog is the multicentric form as described above. There are other forms:
-
Skin form (also called mycosis fungoides)
-
Gastrointestinal form (affecting only the GI tract)
-
Leukemia (bone marrow form)
Lymphoma can occur anywhere in the body where there is lymph tissue. At this time, I will concentrate on multicentric lymphoma.
Chemotherapy
The word chemotherapy conjures images of the bald Elizabeth Perkins from The Doctor or the bald and vomiting Campbell Scott in Dying Young. It is unfortunate that many pets (and probably people, too) do not receive chemotherapy based upon these unpleasant images that do not truly represent the current state of treatment response. Chemotherapy simply means therapy using medication, as opposed to therapy using surgery or radiation. We hope that you will open your mind to what decades of research and clinical experience tells us about chemotherapy rather than listening to what Hollywood has to say on the subject. The following are common questions pet owners commonly have regarding chemotherapy for their dog.
My dog is not acting sick in any way. Shouldn’t I wait until she at least feels sick before beginning chemotherapy?
This might seem like a reasonable approach at first glance but let us assure you that it really isn’t. One of the most important factors in determining the quality of remission (i.e., how fast we get remission and how long it lasts) is whether or not the patient is feeling sick at the time chemotherapy is started. When lymphoma patients are staged (see above under “does my pet need further tests”), stages are subcategorized as “a” or “b” (for example, a multicentric lymphoma dog who feels well is in stage IIIa while a multicentric lymphoma dog who is vomiting or not eating is in stage IIIb). You will have a much better chance for long term quality survival if lymphoma is treated while the patient is an “a.”
Should we see an oncologist?
It is never wrong to see a specialist. Lymphoma is such a common malignancy in humans that there are always new drugs, new protocols and experimental therapy that your regular veterinarian may not be familiar with. Seeing a specialist may be the best way to present you with all of your options. If you are interested, ask your veterinarian for a referral.
Will chemotherapy make my dog sick?
Probably not. Nausea or infection are possibilities but most dogs do not experience any such complications. Only 7% of patients require hospitalization due to side effects of chemotherapy. The bottom line here is to know that animals rarely get sick from chemotherapy but that you should know what to do in case of a problem (see later)
Will chemotherapy make my dog lose his hair or go bald?
While whiskers are commonly lost, substantial hair loss is not experienced by animals on chemotherapy for cancer. There are some notable exceptions: breeds that have synchronous hair follicle activity. Most breeds have hairs in all diffferent stages of the growth-shed cycle at the same time. A few breeds have all hairs in the same stage of growth-shed at the same time. The breeds that can have a baldness issue include: the Olde English Sheepdog, the poodle, the lhasa apso, the shih tzu.
How will I know when we have achieved remission?
A patient in remission is indistinguishable from a completely cancer-free patient. The lymph nodes will go down to normal size and if there were any signs of illness related to the cancer, these should resolve. There is approximately a 75% chance of achieving remission regardless of protocol selected.
How will I know when we have lost remission?
The most obvious sign will be that the lymph node enlargement has returned. This means that the cancer is now resistant to the drugs being used and new drugs must be chosen. (This is called a rescue.)
How long will my dog have quality life on chemotherapy?
This depends on what protocol you choose and there are many. There are also many factors that influence how an individual will do relative to the “average” response. Important parameters to note when reviewing a protocol are: 1) the disease-free interval (i.e., how long the patient is free from illness); 2) survival time; 3) typical duration of remission; 4) expense; and 5) scheduling. |
|

|
|
Protocols and Studies
Combination chemotherapy with L-asparaginase, lomustine, and prednisone for relapsed or refractory canine lymphoma: Saba, C.F., Thamm, D.H., Vail, D.M. Journal of the American College of Veterinary Internal Medicine. Jan/Feb 2007; 21: 127-132.
This study looked at 31 dogs with the multicentric form of lymphoma, all of whom had either relapsed after the CHOP (cyclophosphamide/doxorubicin/vincristine/prednisone) protocol or did not respond to it in the first place. Of these dogs, 52% achieved remission and overall 87% showed at least some response. The median time to achieve a response was 3 weeks. For dogs achieving remission, the disease began to progress again after a median of 111 days. For dogs achieving only a partial response, disease began to progress again after a median of only 42 days). Side effects
occurred in most dogs but were described as mild and generally required no treatment.
Chemotherapy followed by half-body radiation therapy for canine lymphoma: Williams, L.E., Johnson, J.L., Hauck, M.L. Ruslander, D.M., Price, G., and Thrall, D.E.
Journal of the American College of Veterinary Internal Medicine. Sept/Oct 2004; 18: 703-709
Half-body radiation involves irradiating the front of the dog's body two days in a row, waiting 3 weeks, and then irradiating the rear half of the dog's body for two days in a row. In this study 94 dogs with lymphoma received an 11 week chemotherapy induction using
prednisone, L-asparaginase, vincristine, doxorubicin, and
cyclophosphamide. Of the 94 dogs receiving chemotherapy, 78% (73 dogs) achieved remission. Of these 73 dogs, 52 underwent half-body radiation as above. Only dogs that had achieved remission were allowed to have radiation. The median remission time for these 52 dogs was 311 days. Thirty-one of these 52 dogs lost remission during the time of the study and twenty of them repeated chemotherapy induction, followed by maintenance chemotherapy (without more radiation). Seventeen out of twenty were able to achieve a second remission. It is not entirely clear whether or not this protocol increased the median remission duration over more routine chemotherapy but the relatively short (11 week) chemotherapy protocol may provide substantial convenience factor for an owner. Another important advantage was the fact that 85% of dog seeking a second remission were able to obtain one. The disadvantage of this protocol is the expense of radiation and the fact that the necessary equipment may not be readily available.
By Wendy C. Brooks, DVM, DipABVP
Educational Director, VeterinaryPartner.com
Web Site |
|

|
| |
|
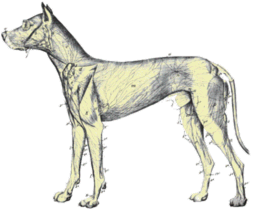
What is the Lymph System?
|
|
Picture taken from Miller’s Anatomy of the Dog, Second Edition. W.B. Saunders Company.
The lymph system is represented by a network of lymphatic vessels and lymph nodes through which foreign proteins and disease organisms are circulated. The lymph nodes serve as immune system centers where these foreign substances may be presented to the cells of the immune system. There are many different types of immune-related cells; some produce anti-bodies, some circulate and destroy the foreign materials they encounter, some regulate the activity of other cells.
Lymphocytes are the primary cells of the lymph system and they act in the various ways mentioned. The lymph vessels serve as a circulatory path for lymphocytes in addition to serving as a collection system directing foreign substances toward the lymph nodes. Lymph vessels interface with the blood stream at several areas allowing lymphocytes greater area to patrol. |
|
|

|
|
WORDS YOU DON'T WANT TO HEAR |
|
|
|
Osteosarcoma and Lymphoma: two words you hope to never hear coming from your veterinarian. Osteosarcoma (bone cancer) and
Lymphoma (a disorder of white blood cells) are the most common types of cancer in dogs. But thanks to the efforts of two veterinary oncologists at the University of Illinois, Veterinary Teaching Hospital in Urbana, these evil enemies of our four legged family members have a tough battle ahead.
As cancer cells are rapidly attacking, Dr. Timothy Fan, an assistant professor, and Dr. Laura Garrett, a clinical assistant professor, are working hard at the University of Illinois College of Veterinary Medicine to investigate novel treatment options and stay one step ahead of our pet's arch rivals. "The positive aspect of this situation is that these common cancers, especially lymphoma, are very responsive to systemic chemotherapy treatment, but as time progresses surviving cancer cells inevitably become resistant to our traditional therapies, and we hit a brick wall," says Dr. Fan.
Dr. Garrett is leading a clinical research trial with canine lymphoma. She is currently working with Dr. Paul Hergenrother in the University of Illinois Department of Chemistry to test the safety and effectiveness of a revolutionary small molecule that possesses the capacity to preferentially cause tumor cells to die. Dr. Fan's research focuses on the treatment of osteosarcoma. He is collaborating with Dr. Jianjun Cheng, a researcher from the Department of Material Sciences and Engineering to evaluate the clinical usefulness of a very small bead (using nanotechnology) that holds chemotherapy drugs that specifically target the bone microenvironment in which cancer cells grow.
According to Dr. Fan, osteosarcoma is usually seen in dogs older than seven, and the disease has a higher incidence in certain breeds, such as
Rottweilers. "It is important to treat the disease as soon as you observe it to help maintain a reasonable quality of life," says Dr. Fan. The typical symptoms of a dog with bone cancer are sudden onset of lameness that becomes extremely painful. Radiographs, or x-rays, are performed to support a diagnosis, but the only way to confirm ostesarcoma is with a biopsy, or aspirate of the tumor.
There are two general treatment plans for bone cancer: pain management, or the best the veterinary profession can offer at this point -- amputation and chemotherapy. According to Dr. Fan, pain management alone will not stop the growth of the tumor, nor prevent it from spreading to other parts of the body. But it will give your pet approximately another 4-6 months of quality life.
The other option, amputation of the affected limb, followed by systemic chemotherapy, buys you a bit more time. "Fifty percent of dogs who undergo this treatment will live a year, and twenty percent live two years," says Dr. Fan.
It is important to note that although this therapy will not be inexpensive, animals tolerate chemotherapy much better than humans because the dose given is significantly less. Only a minority of animals experience adverse side effects, mentions Dr. Fan.
Despite the best efforts of researchers across the country, treatment of cancer in animals has still not caught up with humans. The biggest impediment is finances because most families opt not to carry health insurance for their pets.
Secondly, there are a very limited number of clinics in the country with the infrastructure to treat dogs aggressively. Because of researchers like Drs. Fan and Garrett, there is hope that the thousands of dogs
diagnosed with osteosarcoma or lymphoma may live a longer and better life.
For more information about cancer in pets, contact your local veterinarian.
Ashley Mitek
Information Specialist
University of Illinois
College of Veterinary Medicine
Web Site |

|
| LINKS TO ARTICLES ON OTHER SITES |
|
|
|
| |

|
|
|