|
The immune system is the surveillance and
defence system of the body. It recognizes foreign substances (those not belonging to the body, e.g., viruses, bacteria, pollen) by their molecular features and eliminates them from the body.
| Two functional divisions of the immune system (innate and adaptive)
The immune system can be divided into two parts based on how specific their functions are. These two divisions are called the innate immune system and the adaptive immune system.
Innate immune system: All organisms, even trees, have what could be considered an innate
defence system. For trees it would be their bark, for dogs and cats it would be their skin, and for a bacterium it would be the cellular wall around it.
The innate immune system is the first line of defence. It is non-specific, meaning it is designed to more or less keep everything out. And it is nonadaptive, meaning its effectiveness is not changed by repeated exposure to a foreign substance. In addition to the skin, stomach acid, mucous in the respiratory system, and special chemicals in saliva are part of this innate system. There are also certain cells in the body called phagocytes (eaters) and include cells called monocytes and macrophages (literally, 'big eaters'). These cells will basically eat anything foreign that is in sight.
 A medieval castle would be a good analogy of the innate immune system. The high castle walls and the moat around the castle are designed to keep almost everything out. They act like the body's skin, mucous, and stomach acid. In the moat, we have alligators, which like the macrophages in the body, will basically eat anything. A medieval castle would be a good analogy of the innate immune system. The high castle walls and the moat around the castle are designed to keep almost everything out. They act like the body's skin, mucous, and stomach acid. In the moat, we have alligators, which like the macrophages in the body, will basically eat anything.
Adaptive immune system: In addition to the innate system, dogs, cats, and other animals including humans have an adaptive immune system. The adaptive system defends the body against specific foreign invaders, designing different tactics for different invaders. The parts of the adaptive system communicate with each other and develop a memory of the various invaders they encounter.
In our castle analogy, the adaptive immune system would include archers, spear-throwers, cannoneers, and swordsmen. They each use different tools and defend against those invaders for which they are best designed. They remember previous battles and can improve the speed and efficiency in which they defend the castle.
 Working
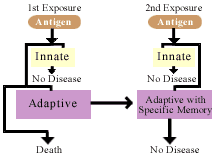
together: The innate system is the first line of defense. If the invader is stopped by the innate system, no disease will occur. If, however, the invader cannot be stopped by the innate system, the adaptive system is activated. If the adaptive system is successful, the body will recover. The adaptive system will also retain memory of the invader. So, if a second exposure to the invader occurs, the adaptive system will mount a greater and faster response, usually preventing disease. If neither the innate or adaptive systems are effective, death can occur. Working
together: The innate system is the first line of defense. If the invader is stopped by the innate system, no disease will occur. If, however, the invader cannot be stopped by the innate system, the adaptive system is activated. If the adaptive system is successful, the body will recover. The adaptive system will also retain memory of the invader. So, if a second exposure to the invader occurs, the adaptive system will mount a greater and faster response, usually preventing disease. If neither the innate or adaptive systems are effective, death can occur.
|
|
Cells of the immune system
As we learn more about how the immune system works, it will help to have a better understanding of the players. The cells of the immune system all start out in the bone marrow, but mature along different pathways.
Monocytes and macrophages: When mature, monocytes and macrophages leave the bone marrow and spread throughout the body. Monocytes generally stay within the bloodstream. Macrophages enter the tissues and do their work there.
As part of the innate immune system, the phagocytose (eat), digest, and kill foreign invaders. They can also serve as part of the adaptive system by presenting portions of the invaders (the antigens) to other cells in the adaptive system, alerting them to the presence of the invader.
Granulocytes: There are several different types of granulocytes, which differ in function and in appearance when stained with certain stains in the laboratory. They mature in the bone marrow and then circulate in the blood and also enter tissues. They are also phagocytes, and are part of the innate system.
Lymphocytes: Lymphocytes have a life cycle similar to animals. They are 'born' in the bone marrow. As they mature, they are 'educated.' Some of them go to the thymus gland (different than the thyroid gland) and are educated there. These are called 'T cells' - 'T' for 'thymus.'
The other lymphocytes are educated in a different area. In the chicken, the area is called the 'bursa' and so these are called 'B cells.' In birds, the bursa is a modified piece of intestine. Mammals do not have a bursa, but instead cells either go to the fetal liver or remain in the bone marrow to be educated. So the 'B' in 'B cell' could also stand for 'bone marrow.'
Once educated, both the B and T lymphocytes are then employed and move throughout the body to where the jobs are. They tend to accumulate in the lymph nodes and spleen. We will talk more about the education of lymphocytes below.
The immune response
What are antigens? Antigens are molecular structures on the surfaces of such particles as bacteria, viruses, and pollens. Antigens are recognized by the body as 'foreign' and stimulate the body to defend itself against them. Antigens have various sizes and shapes. They also have a specificity. That is, all of a certain type of bacteria, virus or other foreign substance (e.g., pollen) will have the same, or almost identical antigens. A virus generally has several different kinds of antigens on its surface. The same is true for bacteria, parasites, pollens, etc.
Education of lymphocytes and recognition of
antigens: Each lymphocyte, whether a B cell or a T cell is educated to identify one particular antigen which has a certain shape and size. The educated B and T cells use antigen receptors on their surface to recognize antigens. The antigen and the receptor fit together like a lock and key. Some lymphocytes will only have receptors for a certain antigen (let us call it A1) on a parvovirus. Other lymphocytes will only have receptors for a hypothetical A2 antigen on the parvovirus. (The body may recognize many different antigens on one invader and respond to each of them.) Another population of lymphocytes has receptors for specific antigens on a Salmonella bacterium. Still others only recognize a certain antigen on grass pollen. When you think about it, this is truly amazing. There are literally millions of antigens in the world, and mammalian bodies produce different lymphocytes which recognize each antigen.
The cells of the animal's body also contains antigens. The B and T cells are taught to ignore these and regard them as 'self'. The various blood types in people: A, B, AB, and O result from different antigens on the red blood cells. People with Type A blood have 'A' antigens on their red blood cells; people with Type B blood have 'B' antigens. The B and T cells of people with blood type A do not see the 'A antigen' as foreign, but the T and B cells of a person with blood type B would.
The B cell response, antibodies, and humoral
immunity: When the receptor on a B cell recognizes and attaches to the antigen it was 'designed for' (again, we will use the hypothetical A1), it is a signal to the B cell to start mounting a
defence. The B cell makes molecules called antibodies, which are small disease-fighting proteins. B cells which produce antibodies are also called 'plasma cells.' Antibodies are sometimes referred to as 'immunoglobulins.' The antibodies have receptor areas on them which will bind to the A1 antigens. These receptors are called 'antigen binding sites.' There are two antigen binding sites on each antibody. The antigen and antibody bound together is called an 'immune complex.'
The antigen binding sites are not 100% specific. This means that although the antibody was produced in response to one antigen, in this case Antigen1, it may also be able to bind with other antigens, e.g., Antigen2. You can see how this may happen if you have ever put a puzzle together. You usually can find several pieces that are a close fit, but there is only one piece that really fits. Antigen receptors can sometimes bind with antigens that are close fits, instead of the one antigen they were designed for. When this occurs it is called a 'cross-reaction.'
Cross reactions can be a problem when performing laboratory tests. Let us say you are testing the blood of an animal to see if it has antibodies to our hypothetical A1. Let us also say that antibodies to an antigen we will call B1 (which is from an entirely different organism) will also bind to antigen A1. If the blood of our animal has antibodies to A1, the test will be positive. But, if the blood does not contain antibodies to A1, but does contain antibodies to B1, the test will also look positive. But in this case it is falsely positive.
In the body, the binding of the antigen by the antibody can result in:
-
Neutralizing a toxin if the antigen was on a toxin
-
Deactivating a virus if the antigen was on a virus
-
Activating a cell-killing series of proteins called 'complement'; antibody and complement together can lyse (break apart) bacteria and kill them
-
Making the antigen (and what it is attached to) more appealing to phagocytes. This is called opsonization. Antibody bound to the antigen is like mustard on a hot dog - the phagocytes will eat it with more relish.
The T cell response and cell-mediated
immunity: When the receptors on a T cell bind to an antigen it activates the T cell. Some T cells will bind to the foreign invader carrying the antigen and destroy it. Other T cells will become activated and make substances called lymphokines. These are chemical messengers to the macrophages and other phagocytes, calling them to "come in and eat."
Memory: Whether the body's response is primarily humoral (through antibodies) or cell-mediated, certain T and B cells become 'memory cells.' These cells remember their exposure to the specific antigens which were on the foreign substance. This is the mechanism by which vaccination helps protect the body from disease. If a dog, for instance receives a combination vaccine containing distemper, hepatitis, and parvovirus, 3 different groups of memory cells will be produced: one group will remember the distemper antigens, another will remember hepatitis antigens, and the third group will remember the parvovirus antigens.
These memory cells help the body respond much faster and with a larger response, if they are ever again exposed to the antigen for which they have memory. For example, if the dog above was vaccinated against distemper, and then 3-4 weeks later vaccinated against distemper, the body's response to the second vaccination will be greater and much faster than after the first vaccination. This faster and higher response is scientifically termed a
'secondary response' or an 'anamnestic response.' This more efficient response is due to the memory cells. These memory cells are not produced instantly. The time period between exposure to the antigen (either through vaccination or an infection) and the creation of memory cells is generally 2-3 weeks.
The memory cells 'prime' the body in case of a subsequent exposure to the antigen. We have all heard of 'priming the pump.' An unprimed pump will take a lot of strokes of the pump handle before it produces any water. A primed pump, however, may produce a good deal of water on the first stroke. A 'primed' immune system will react more swiftly, just like a primed pump.
The memory cells created against some diseases live a long time, while those for other diseases may have a relatively shorter life span. Since memory cells do not live forever, in some cases, we need to revaccinate an animal to produce a new generation of memory cells. For some diseases this is every year, for others 3 years or longer. When we talk about duration of immunity (length of time an animal is protected), we are really talking about how long a sufficient number of memory cells live, and how long the antibodies remain so that the animal is still protected.
Two ways to acquire immunity (active and passive)
There are two main ways in which an animal can acquire immunity.
Active immunity: When people or animals are exposed to a disease-causing organism by natural means or vaccination, the antigens on the organism interact with the cells of the animal's immune system. The B cells make antibodies to destroy the organism. T cells are activated and also help to eliminate the organism. When an individual has an immune system that will effectively protect it against a disease-producing organism, it is said to have immunity to that organism. When an animal’s own immune system provides that protection, it is referred to as 'active immunity.'
Passive immunity: When an animal receives another animal's
defence mechanisms (antibodies and/or lymphocytes), rather than developing its own
defence system, we refer to it as 'passive immunity.' Examples of passive immunity include the antibodies received by a fetus through the placenta, antibodies the newborn receives from its mother through
colostrum, antivenins to treat snakebite, and bone marrow transplants which help replace the lymphocytes. A disadvantage of passive immunity is that the animal's body does not have the ability to replenish it (except in the case of a bone marrow transplant). As the antibodies which the animal received break down through natural aging, or are used up destroying disease-causing organisms, the animal's body cannot replace them. However, in the case of active immunity, more antibodies are produced whenever the immune system comes in contact with the same organism again. Active immunity is self-perpetuating. Passive immunity is not.
Abnormalities of the Immune System
The immune system does not always function properly. Sometimes, it reacts to the wrong thing (autoimmunity), other times, it reacts too much (hypersensitivity), and sometimes it simply does not react at all (immunosuppression and immunodeficiency).
Autoimmunity: In autoimmunity, the immune system mistakenly sees some part of the body as foreign and starts to attack it. Both the T cells and B cells may be involved in autoimmunity. What causes autoimmunity?
Genetics may play a role in the development of some types of autoimmunity. An autoimmune disease called systemic lupus erythematosis (often just spoken of as 'lupus'), is more common in German Shepherds than many other breeds.
Certain drugs may alter the molecular appearance of cells. Some drugs attach themselves to red blood cells, making the cells appear 'foreign.' The body then attacks the red blood cells causing autoimmune hemolytic anemia.
As with certain drugs mentioned above, in some cases, antigen-antibody complexes may adhere to cells and cause the same type of phenomenon - the body attacks the cells since they appear foreign. In some cases, a great deal of inflammation can accompany the killing of these cells. This type of autoimmune reaction is thought to contribute to rheumatoid arthritis.
Errors in the 'education' of T and B cells may make them unable to distinguish 'foreign' from 'self.'
Many researchers are exploring the various aspects of autoimmunity and how it may differ between species of animals. In the future, we hope to have a better understanding of this condition and how we can prevent and treat it.
Autoimmune diseases are classified into two types: those in which the antibodies are directed at a certain organ, and those in which multiple areas of the body are affected.
Hypersensitivity:
A hypersensitive immune system is one which overreacts to a stimulus. In addition to T cells and B cells, various other cells can also be activated during an immune response. These cells produce chemicals such as histamines which can affect multiple parts of the body. In hypersensitivity, the body produces too much antibody, the wrong kind of antibody, a large number of antigen-antibody complexes, or antibody to proteins which are not really foreign. In addition, an excessive number of cells may be activated to produce histamine and other chemicals. There are four major types of
hypersensitivity.
Immunosuppression and immunodeficiency: Certain drugs and disease-causing organisms can suppress the immune system. For organ transplantation and in some cases of autoimmune disease, we want to suppress the immune system and use various drugs to achieve that goal. In some infections with parasites such as malaria,
trichinosis, and
leishmaniasis, the organism can suppress the immune system through various mechanisms, allowing the organism to grow and multiply within the person or animal. Immunodeficiency can occur as a result of a genetic defect in different breeds of cats and dogs. Some viral infections (e.g., feline immunodeficiency virus and canine parvovirus) can cause immunodeficiency, as well. Newborns who did not receive adequate amounts of colostrum are immunodeficient and in great danger of becoming seriously infected with a number of diseases. Poor nutrition, such as Vitamin A, Vitamin E, and selenium deficiencies, and restricted protein or calories can result in suppression of the immune system.
Summary
The immune system is an incredible defense mechanism which protects the body from many kinds of disease-causing agents including bacteria, viruses, toxins, and parasites. The innate portion of the immune system, including the skin, is the first line of defense, is nonspecific, and provides protection from many foreign invaders. The adaptive portion of the immune system is much more specific, reacts to unique molecules called antigens, and uses antibodies and cell-mediated immunity to rid the body of foreign substances. The adaptive portion of the immune system can 'remember' previous encounters with a foreign substance and react faster and to a higher degree with subsequent exposures. A body may acquire immunity through transfer from another animal (passive immunity), or through its own exposure and reaction to a foreign substance (active immunity). Sometimes, the immune system can malfunction and either attack its own body (autoimmunity), overreact (hypersensitivity), or react insufficiently (immunodeficiency or suppression).
Holly Nash, DVM, MS
Veterinary Services Department, Drs. Foster & Smith, Inc.
Web Page |